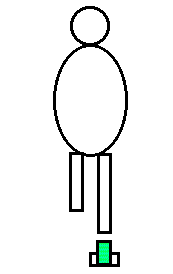- Tape measure
- Text (1 copy of each)
- Hertling, D., & Kessler, R. M. (1996). Management of common musculoskeletal disorders: Physical therapy principles and methods. (3rd ed.). Philadelphia: J.B. Lippincott.
- Kendall, F.P., McCreary, E.K., & Provance, P.G. (1993). Muscles: Testing and Function (4th ed.). Baltimore: Williams & Wilkins.
- Smith, L.K., Weiss, E.L. & Lehmkuhl, L.D. (1996). Brunnstrom's Clinical Kinesiology (5th ed.). Philadelphia: F.A. Davis.
Read pp. 387-392, 401-410 - Anatomy text of your choice
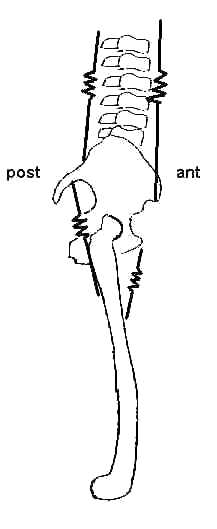
- This course's objectives do not require knowledge of the relative freedom of movement in different spinal regions (Smith, Weiss, & Lehmkuhl, 1996, Fig. 11-3, p. 373). Still, you should take a few minutes to review vertebral anatomy, attending specifically to the orientation of the facet (zygapophyseal) joints. These joints' orientation helps determine an intervertebral joint's relative range of motion in the three planes. For example, the lumbar facet joints' flat surfaces lie primarily in the sagittal plane. Accordingly, flexion and extension are relatively free in the lumbar spine, while rotation is relatively less free.
In contrast, the thoracic facet joints are oriented more obliquely, so thoracic movement is more equal among the three planes. Thoracic sidebending is relatively limited (Smith, Weiss, & Lehmkuhl, 1996, Fig. 11-3, p. 373), not because of the facet joints' orientation but because of the presence of the ribcage.
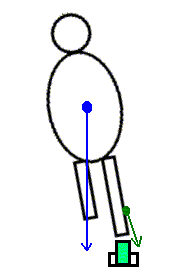
- Begin a postural assessment by standing behind one of your lab partners as he or she stands barefoot. View your partner's right and left feet from behind, and compare the angulation of the Achilles tendons where they insert on the calcanei. Do the angles indicate that the calcanei are:
- inverted? This alignment is also called calcaneus varus or rearfoot varus, and a component of subtalar supination.
- everted? This alignment is also called calcaneus valgus or rearfoot valgus and is a component of subtalar pronation.
- Ask your lab partner to rotate the pelvis in the transverse plane. Although this maneuver is not part of a typical postural assessment, it permits you to note the subtle changes that occur in the calcaneal alignment as the pelvis rotates.
- The calcaneus moves toward inversion on the side that the pelvis moves backward. Calcaneal inversion is a component of subtalar supination.
- The calcaneus moves toward eversion on the side that the pelvis moves forward. Calcaneal eversion is a component of subtalar pronation.
- Compare the level of the right and left ASIS in the frontal plane. Do this by kneeling behind your lab partner and palpating the ASIS with your hands at the level of your shoulders. Decide whether the pelvis is level by using your proprioceptive sense more than your vision. You may prefer to close your eyes.
Stand and, placing your your hands on your partner's right and left shoulders, assess their relative height.
If you find that the pelvis is not level, investigate the source of the asymmetry.
- Is one subtalar joint more pronated than the other? When the subtalar joint pronates, it permits the talus to move inferiorly, flattens the foot's longitudinal arch, and decreases the functional length of the respective lower limb. You might trace an unlevel pelvis to an asymmetry between the right and left subtalar joint postures.
- If the subtalar joints appear to be symmetrical, are the popliteal creases at the same height? Perhaps one knee is hyperextended, making the leg functionally longer.
- If the popliteal creases are level, are the greater trochanters symmetrical? Relative flexion or rotation of one hip may contribute to the assymetrical pelvic position.
- If you cannot find a functional source for the pelvic asymmetry, you should consider a structural leg length difference. One of your texts (Hertling & Kessler, 1996, p. 298) refers to an accurate tape measure test. In this test (Beattie, Isaacson, Riddle, & Rothstein, 1990, p. 153) the subject is supine with the hips in neutral rotation and the malleoli close together at the body's midline. The examiner stands on the side of the leg being measured, and stretches a tape measure from the inferior border of the ASIS to the inferior border of the medial malleolus.
The measurement technique is described in:
Beattie, P., Isaacson, K., Riddle, D.L., & Rothstein, J.M. (1990). Validity of derived measurements of leg-length differences obtained by use of a tape measure. Physical Therapy, 70, 150-157. - As your lab partner bends forward, look along the contour of the trunk to check for a "rib hump," evidence that the ribs protrude posteriorly on one side of the spine. The presence of a rib hump is evidence of rotation in the thoracic spine. Because spinal rotation and sidebending are coupled motions in the spine, the presence of rotation is evidence of sidebending. A "sidebent" or laterally flexed spinal posture is called scoliosis.
Scoliosis can be structural or functional. If it is functional, the scoliosis (and its signature rib hump) should disappear when the pelvis is level. To find out if the scoliosis is functional, repeat the forward bending test with your patient seated on a hard surface. If the rib hump persists, the scoliosis may be structural, that is, related to asymmetries or abnormalities in the spine's bony structure.
- Observing your lab partner from the side (in a sagittal plane view) and, using your texts (Kendall, McCreary, & Provance, 1993, p.83; Smith, Weiss, & Lehmkuhl, 1996, p.405) for guidance, visualize the line of application of gravity as it acts on the body.
You can relate your partner's posture to the figures in Muscles: Testing and Function that begin on page 84. However, we don't fully understand the reliability of this system for naming postures.
- Note your partner's lumbar lordosis. Ask your partner to change the lordosis, without moving the upper trunk, by moving the pelvis.
Identify trunk and hip muscles whose activity tilts the pelvis anteriorly or posteriorly, and thereby alters the lumbar spine's posture in the sagittal plane.
anterior pelvic tilt: a sagittal plane motion that causes the ASIS to move anteriorly. posterior pelvic tilt: a sagittal plane motion that causes the ASIS to move posteriorly.
- The modified Schober method: a technique for assessing spinal motion. Although the technique is reliable (Moll & Wright, 1971), its primary usefulness may be in screening for the very limited mobility that patients exhibit who have diseases like ankylosing spondylitis.
Use a pen to mark the midpoint between the posterior superior iliac spines (PSIS). Then use your tape measure to identify and mark two points: (1) one that is 10 cm superior to the PSIS, and (2) one that is 5 cm inferior to the PSIS.
As your partner flexes the spine as far as possible, measure and record the distance between the superior and inferior marks.
Similarly, measure and record the distance between the superior and inferior marks as your partner extends the spine as far as possible.
Lab partner
Distance (in cm) during flexion
Distance (in cm) during extension
1 2 3 4 This modification of the Schober test is published in:
Cole, B., Finch, E., Gowland, C., & Mayo, N. (1995). Physical rehabilitation outcome measures. Baltimore: Williams & Wilkins. Moll, J.M., & Wright, V. (1971). Normal range of spinal mobility: An objective clinical study. Annals of the Rheumatic Diseases, 30, 381-386.
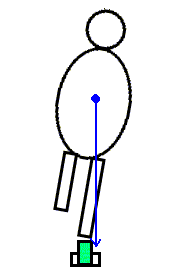
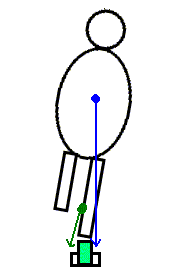
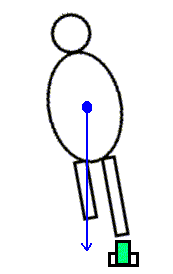
- Balance and posture in single limb stance
As your lab partner stands barefoot on one leg (with the eyes closed), observe and palpate the tendons of the extrinsic foot muscles, which cross both the ankle and subtalar joints. As the person "sways" over the base of support, and the line of application of gravity moves anteriorly or posteriorly, medially or laterally, how does it affect the ankle and subtalar joints. Which muscles activate to counter gravity's effects on the two joints?
After you've considered this problem, you can consult a commentary that addresses it.
Commentary on "Balance and posture in single limb stance"